Updated on Jun 30, 2022 | Community, Featured

Lisa M. Satlin, MD, Pediatrician-in-Chief, Kravis Children’s Hospital at Mount Sinai, with Alfin G. Vicencio, MD, Chief, Pediatric Pulmonology, left, and Jeffrey M. Saland, MD, MSCR, Chief, Pediatric Nephrology and Hypertension.
Kravis Children’s Hospital at Mount Sinai has again been ranked among the nation’s top children’s hospitals by U.S. News & World Report in its “Best Children’s Hospitals” guidebook for 2017-2018.
Mount Sinai ranked in six of ten specialties and achieved top 25 rankings in two specialties—Diabetes & Endocrinology, and Gastroenterology & GI Surgery. Three departments improved their rankings over the previous year. The rankings, published annually, recognize the nation’s top 50 children’s hospitals in 10 pediatric specialty areas.
Committed to providing exceptional care to children and their families, Mount Sinai has created an alliance with the Children’s Hospital of Philadelphia (CHOP), one of the nation’s leading children’s hospitals. Patients in the New York metropolitan area now have access to CHOP specialists in fetal medicine, pediatric cardiac care, and pediatric oncology—and to the most advanced diagnostics and treatments from Mount Sinai and CHOP experts—close to home at select Mount Sinai locations.
“This year’s rankings reflect the excellent care provided to our pediatric patients and their families,” says Kenneth L. Davis, MD, President and Chief Executive Officer of the Mount Sinai Health System. “We are grateful to each one of our employees—from the physicians and nurses to the social workers and staff—for making this recognition possible through their tireless work.”
The national rankings were generated from data collected through a clinical survey sent to nearly 200 hospitals that measured areas such as patient safety, infection prevention, and nurse staffing. Part of each hospital’s score is also derived from a reputational survey that went to about 11,000 pediatric specialists who were asked to name up to 10 hospitals they consider best in their specialty for children with serious or complex medical issues.
“We continue to recruit renowned experts to our medical teams, and the excellence we have achieved at Kravis Children’s Hospital is reflected in these rankings,” says Dennis S. Charney, MD, Anne and Joel Ehrenkranz Dean, Icahn School of Medicine at Mount Sinai, and President for Academic Affairs, Mount Sinai Health System. “Innovative programs, such as our partnership with Children’s Hospital of Philadelphia, will expand access to unparalleled care for children in the New York area.”
The hospital, which sees more than 70,000 outpatient visits and 3,000 inpatient stays each year, is ranked in the following specialties:
- Diabetes & Endocrinology No. 16, up from No. 38
- Gastroenterology & GI Surgery No. 23, up from No. 27
- Neurology & Neurosurgery No. 27, up from No. 30
- Urology No. 30
- Pulmonology No. 32
- Nephrology No. 39
The Pediatrician-in-Chief of the Kravis Hospital is Lisa M. Satlin, MD, Herbert H. Lehman Professor and Chair, Jack and Lucy Clark Department of Pediatrics, Icahn School of Medicine at Mount Sinai. “Every day, our doctors, nurses, child-life specialists, and our entire staff aim to ensure that every patient receives the best possible care, leading to the best possible outcomes, in a supportive environment that is focused on each individual child and his or her family,” says Dr. Satlin.
Jul 11, 2017 | Community, Featured

Seated: Barbara J. Niss and Arthur H. Aufses, Jr., MD. Back row, from left: Carolyn Aufses Blashek, Harriet Aufses, and Arthur H. Aufses III.
The Mount Sinai Health System’s archives, housed in a simple suite of offices on the Icahn School of Medicine at Mount Sinai campus, belies the rich trove of historical documents belonging to seven storied hospitals that are preserved inside.
Filed in these archives is an article about medicine as a noble calling that was written in 1848 by Woman’s Hospital physician E. Randolph Peaslee, MD. (The Woman’s Hospital was later merged into Mount Sinai St. Luke’s.) There are also minutes from the first board meetings for St. Luke’s Hospital from 1850, and for The Jews’ Hospital in 1852 (renamed The Mount Sinai Hospital in 1866), and the minutes from Mount Sinai Beth Israel’s founding board meeting in 1889 that were written in Yiddish.
These documents and many others from Roosevelt Hospital—renamed Mount Sinai West in 2015—and a limited collection from New York Eye and Ear Infirmary of Mount Sinai, Mount Sinai Queens, and Mount Sinai Brooklyn, provide unique glimpses into New York City’s history and how the practice of medicine has evolved over the centuries.
“History is many stories. We try to bring these stories to people at Mount Sinai so they will know and appreciate them,” says Barbara J. Niss, Director, The Arthur H. Aufses, Jr. MD Archives and Mount Sinai Records Management Program, part of the Academic Informatics and Technology Department. “The more you know about a place, the more connected you feel to it.”
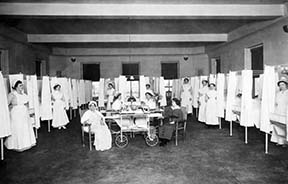
The women’s ward at Mount Sinai St. Luke’s circa 1900.
Upon request, Ms. Niss provides one-hour historical walking tours of The Mount Sinai Hospital (MSH). The Archives’ staff also creates quarterly displays in the Annenberg North Lobby on historical topics using the Archives’ records. The Mount Sinai archivist since 1986, Ms. Niss co-wrote the definitive history of MSH and its clinical and surgical accomplishments in the book
This House of Noble Deeds: The Mount Sinai Hospital, 1852-2002, with Arthur H. Aufses, Jr., MD, retired Chairman of the Department of Surgery. She and Dr. Aufses also wrote a history of Mount Sinai’s School of Medicine in 2004.
Over the years, Dr. Aufses and his wife, Harriet, have been strong supporters of Mount Sinai. They established the Aufses Family Scholarship, lectureships in the Departments of Surgery and Population Health Science and Policy, and prizes for surgical residents and students. Dr. Aufses’s Mount Sinai roots date back to 1921, when his father began his surgical training at MSH. He says he first visited the archives in the mid-1980s to look for early surgical cases. “It was an incredible experience to see the vast collection of historical material dating back to the 1850s. I became fascinated with the archives.”
Preserving, organizing, and digitizing the Health System’s archival documents is an ongoing project for the Archives staff, and content is added to the collection daily. (Mount Sinai’s Records Management Program is also based in the Archives.) The staff regularly receives requests for information about a particular medical subject, hospital within the Health System, or individual. Ms. Niss says there is ongoing interest in refugee physicians who arrived in New York after fleeing Nazi Germany, in the history of the Woman’s Hospital, and from the families of women who graduated from three of the hospitals’ former schools of nursing.
The Aufses Archives also provided significant support in establishing the Mount Sinai History Wall, an artistic timeline unveiled in December 2016 that showcases in words and pictures each hospital’s transformative contributions to medicine, science, and patient care over the past two centuries. The History Wall is located on the fourth floor of the Corporate Services Center at 150 East 42nd Street, outside the seminar room where new employees attend orientation on their first day of work at Mount Sinai.
Updated on Jun 30, 2022 | Community, Featured

Graduating residents and fellows in Ophthalmology and Otolaryngology
Faculty, parents, and friends celebrated the accomplishments of 22 residents and fellows in Ophthalmology, Otolaryngology, and Plastic and Reconstructive Surgery at the 2017 Commencement of the New York Eye and Ear Infirmary of Mount Sinai.
James C. Tsai, MD, MBA, President, New York Eye and Ear Infirmary of Mount Sinai, and Chair of Ophthalmology, Mount Sinai Health System, welcomed graduates and guests to the event, held on Thursday, June 22, at the Friends Meeting House.
“It has been a pleasure and a privilege to teach and mentor this extraordinary class. Be proud of your achievements and celebrate your successes,” Dr. Tsai said, setting out goals for the future: “Use your knowledge to lead changes in health care for the better, and deliver exceptional patient care. Challenge the status quo to make a positive difference, seek opportunities to provide global assistance to revive hope. Innovate and dream big.”
Four of the graduates were residents specializing in otolaryngology, and seven were residents in ophthalmology. The residents will now take fellowships at top-tier institutions, including the University of California, San Francisco; Wills Eye Institute in Philadelphia; and Emory University Hospital in Atlanta.
Eleven fellows completed training in subspecialties, including cornea and refractive surgery, glaucoma, ocular immunology, vitreoretinal surgery, and aesthetic plastic surgery.
Updated on Jun 30, 2022 | Community, Featured

Members of the Class of 2017 of the Phillips School of Nursing at Mount Sinai Beth Israel
In a jubilant ceremony, the Phillips School of Nursing (PSON) at Mount Sinai Beth Israel graduated 80 new nurses who received an Associate’s Degree in Nursing, and conferred a Bachelor of Science in Nursing degree to 24 registered nurses. The 113th graduation ceremony was held on Tuesday, June 6, at Stern Auditorium on the campus of the Icahn School of Medicine at Mount Sinai.
Presiding at the ceremony were Janet A. Green and Ruth Nerken, Co-Chairs of the Board of PSON, who presented the degrees. Carleen Graham, MSN, RN, Program Coordinator, RN-BSN Program, served as the Platform Marshall, and Lorraine McGrath, MA, RN-BC, Assistant Dean for Academic Affairs, gave graduates their PSON pin.
Twenty graduates were inducted into the Honor Society, which was founded in 2012. These students successfully achieved a grade point average of 3.7 or higher.
Todd F. Ambrosia, DNP, MSN, RN, Dean, welcomed the graduates, faculty, staff, and guests. The commencement address was given by Betsy M. Tirado-Ortiz, RN. Now retired, Ms. Tirado—a 2016 recipient of the Nurse of the Year Award from the National Association of Hispanic
Nurses—maintains a passion for nursing and continues to participate in a number of international missions that help children with congenital heart defects.
“Don’t waste your time waiting to win the lotto. You have already won the lotto—you are a professional nurse,” Ms. Tirado told the graduates. “Make your own riches, share them, and enrich your own life and the lives of others. You each carry within you the power to go from magical thinking to the power of completion.”
Updated on Jun 30, 2022 | Featured, Your Health

From left: David L. Reich, MD, President and Chief Operating Officer, The Mount Sinai Hospital; Dennis S. Charney, MD, Anne and Joel Ehrenkranz Dean, Icahn School of Medicine at Mount Sinai, and President for Academic Affairs, Mount Sinai Health System; Kenneth L. Davis, MD; Madeline Bell, President and Chief Executive Officer, Children’s Hospital of Philadelphia; and Lisa M. Satlin, MD, Herbert H. Lehman Professor and Chair, Jack and Lucy Clark Department of Pediatrics, Icahn School of Medicine at Mount Sinai.
The Mount Sinai Health System and Children’s Hospital of Philadelphia (CHOP) launched the next phase of their 18-month-old alliance on Wednesday, May 31, as they officially opened their Fetal Medicine Program and announced an affiliation of the Mount Sinai Children’s Heart Center with the Cardiac Center at CHOP. The celebration included a ribbon-cutting ceremony on the third floor of the Annenberg Building—the location of the new Fetal Medicine Suite—that was attended by several dozen leaders and staff from both institutions.
The Mount Sinai and CHOP alliance began in the fall of 2015 and includes three areas: fetal medicine, pediatric cardiac care, and pediatric oncology. In all three areas, the collaboration intends to give patients and their families access to the most advanced diagnostics and treatments by Mount Sinai and CHOP specialists at several Mount Sinai locations.
“We are combining our strengths to give children in the New York metropolitan area access to an unprecedented scope of pediatric services,” Kenneth L. Davis, MD, President and Chief Executive Officer, Mount Sinai Health System, told the guests.
“CHOP is pleased to mark this milestone in the relationship between two health care institutions that are totally dedicated to caring for the health of children and their families,” Madeline Bell, President and Chief Executive Officer of Children’s Hospital of Philadelphia, said. “The alliance continues to evolve and reflects both a shared vision to better serve families in the New York region and a mutual professional respect and admiration between our organizations.”
The Fetal Medicine Program is unique for New York: it allows expectant parents facing a high-risk pregnancy to have a comprehensive fetal diagnosis conducted and then reviewed in full detail with a team of specialists, all in a single day. “By the end of the day, parents will have their questions answered, understand the treatment options, and be equipped to make the best decisions for their families,” said Dr. Davis.

From left: Khanh Nguyen, MD, Professor of Cardiovascular Surgery, and Pediatrics, Icahn School of Medicine at Mount Sinai, and Chief, Pediatric Cardiothoracic Surgery, The Mount Sinai Hospital; Joanne Stone, MD, MS; and Peter Pastuszko, MD.
Ultrasound, echocardiography, fetal magnetic resonance imaging, and all diagnostic testing will be performed at The Mount Sinai Hospital. Images will be read by specialists in fetal radiology at CHOP and Mount Sinai in coordination with Mount Sinai maternal-fetal medicine specialists using telemedicine video links. “In effect, we are building a dream team of fetal medicine,” said Joanne Stone, MD, MS, Director, Division of Maternal-Fetal Medicine, Mount Sinai Health System, and Professor, Obstetrics, Gynecology and Reproductive Science, Icahn School of Medicine at Mount Sinai.
The new pediatric cardiac care alliance includes the Fetal Heart Program, which aims to diagnose congenital heart disease as early as 12-14 weeks gestation using fetal echocardiography. Specialists at Mount Sinai and CHOP would then jointly develop an optimal plan for care. Additionally, the Children’s Heart Center at The Mount Sinai Hospital, overseen by the divisions of Pediatric Cardiology and Cardiac Surgery, and offering a continuum of care from fetal to adult life, will now have access to the expertise of CHOP’s Cardiac Center in areas such as pediatric cardiac intensive care and pediatric cardiothoracic surgery. The Mount Sinai and CHOP teams are able to provide joint expertise at all points of treatment through direct consultation and use of telehealth technology.
“Every day, we are confronted with new babies who depend upon us for life,” said Peter Pastuszko, MD, Chief, Pediatric Cardiac Surgery and Director of Pediatric Cardiovascular Services, Mount Sinai Health System, and Professor, Cardiovascular Surgery, Icahn School of Medicine at Mount Sinai. “Today, we are well equipped to handle a congenital heart defect of any complexity.”

The event featured a videoconference with N. Scott Adzick, MD, Surgeon-in-Chief and Director of the Center for Fetal Diagnosis and Treatment, Children’s Hospital of Philadelphia (CHOP), and Professor of Surgery, University of Pennsylvania School of Medicine, and the CHOP team.
Updated on Jun 30, 2022 | Featured, Psychiatry, Research, Your Health
 The Icahn School of Medicine at Mount Sinai recently opened a new Addiction Institute that will address one of the nation’s greatest health concerns by exploring effective treatments for patients with substance abuse problems.
The Icahn School of Medicine at Mount Sinai recently opened a new Addiction Institute that will address one of the nation’s greatest health concerns by exploring effective treatments for patients with substance abuse problems.
“Bringing science to bear on the development of new therapies has reached the top of the national agenda, and that is where Mount Sinai excels,” says Yasmin Hurd, PhD, the Ward-Coleman Chair in Translational Neuroscience and Director of the Addiction Institute at Mount Sinai.
The Institute will manage therapies for all types of substance abuse. By removing the traditional silos that separate research and clinical care, and unifying all areas of addiction under one umbrella, Dr. Hurd says the Institute is “well positioned to meet the challenges of New York City and the nation.” The Institute will leverage Mount Sinai’s considerable body of research and clinical expertise in neuroscience and behavioral health in order to move the field forward.
According to the 2016 U.S. Surgeon General’s Report on Alcohol, Drugs, and Health, more than 20 million Americans have substance abuse disorders and 12.5 million reported misusing prescription painkillers. Despite decades of expense and effort focused on a criminal justice-based model for addressing substance-related problems, the report acknowledged that addiction remains a public health crisis with economic consequences in crime, health, and lost productivity totaling more than $400 billion annually. Dr. Hurd says the Institute’s collaboration with Mount Sinai’s other specialties such as precision medicine, population health, infectious disease, epidemiology, and genomics will help advance treatments and novel discoveries.
“The Institute’s modernized structure across a large, integrated health system will enable us to approach addiction in a cohesive way,” says Dr. Hurd. “In addition to prioritizing our research based on clinical needs, we want to understand the populations at risk and their patterns of behavior. Addiction is complex and one group cannot do it alone.”

Yasmin Hurd, PhD
An important aspect of the Institute’s work will be dispelling the stigma associated with addiction through greater understanding of the biological and behavioral complexities of substance use disorders. Another goal will be encouraging young clinicians to enter residencies and fellowships in the fields of addiction psychiatry and addiction medicine.
“We want to train the best and the brightest through enhanced clinical and research rigor to elevate the field,” says Dr. Hurd. “Clinical treatments for some addictions have not advanced in 50 years. This and other stigmas can deter young physicians from going into this field. Unless we improve the clinical toolkit available for clinicians we will not be able to change the trajectory of care.”
Decades of scientific studies have established that chronic substance misuse leads to profound disruptions of brain circuits involved in pleasure, reward, habit formation, stress, and decision-making. Repeated drug use alters the expression of genes to ultimately increase or decrease their production of proteins, leading to long-term changes in cellular function and even reshaping of the physical structure of neurons.
“Drugs can change the morphology of cells and induce a cascade of adverse events in the brain,” says Dr. Hurd. The Institute plans to move forward with multiple clinical trials that seek to reverse those disruptions. “Most addicts do not want to be addicted,” she adds. “Addiction can be treated. We need medical therapies that partner with behavioral therapies, and we need to be diverse in our treatment portfolio.”









 The Icahn School of Medicine at Mount Sinai recently opened a new Addiction Institute that will address one of the nation’s greatest health concerns by exploring effective treatments for patients with substance abuse problems.
The Icahn School of Medicine at Mount Sinai recently opened a new Addiction Institute that will address one of the nation’s greatest health concerns by exploring effective treatments for patients with substance abuse problems.